Disability claims are tied to a large population in Canada and the United States. Recent survey data show that about 8.0 million Canadians aged 15 and older live with a disability that limits daily activities.
In the United States, CDC data show that 28.7% of adults have some form of disability. A large number of these individuals eventually move into disability benefits systems or disability insurance claims systems, which puts steady pressure on review processes that are already strained.
That pressure is visible in the numbers. The U.S. Social Security Administration reported that roughly 940,000 Americans were waiting for initial disability determinations by mid 2025. That figure was down from the record backlog of 1.26 million reported in mid 2024, but the system remained heavily burdened.
Wait times also moved in the wrong direction over time. What was about 3.7 months in 2017 became about 7.7 months by August 2024. At the same time, the initial approval rate did not improve. Only 36% of U.S. disability claims were approved in fiscal year 2025, down from around 39% in the prior year.
The Canadian context shows a similar strain in a different form. Many disabled Canadians still face barriers long before a claim is fully processed. Survey findings show that 72% of Canadians with disabilities report facing one or more barriers in daily life. Another 17% report difficulty with online activities such as websites and apps. These numbers matter because claims systems now depend more on digital forms, online submissions, portals, and remote communication.
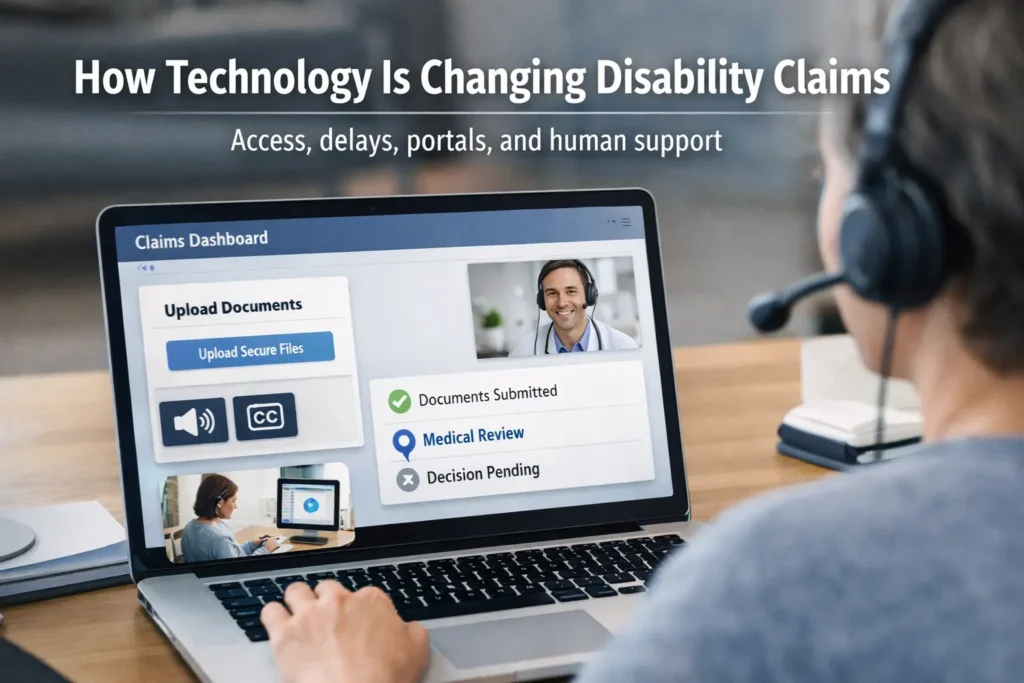
Why Traditional Claims Processing Has Been So Difficult
Traditional disability claims processing has been slow for years because the work is document loaded, medically detailed, and procedurally rigid.
Claimants usually need to collect records, complete forms, secure physician statements, and respond to repeated requests for supporting evidence. A small error in one medical form or one missing attachment can delay a decision for weeks or months.
The process also becomes harder when definitions of disability do not match across systems. A person may have a serious health condition that limits work, but that condition still needs to fit the exact standard used by the insurer or the government program. Incomplete medical forms, unclear physician notes, and rigid administrative requirements add to this problem.
In Canada, the Disability Advisory Committee has pointed to incomplete medical forms and rigid handling of Part B of the Disability Tax Credit form as recurring pain points.
Staffing and process limits also add delay. The SSA’s own review has linked backlog conditions to uneven staffing and outdated processes.
When the volume of files rises, and the number of trained reviewers does not keep pace, every step slows down. Technical issues then make matters worse. A missing electronic file, a portal error, or a document upload problem can hold a claim in place even when the claimant already did the required work.
The Technologies Now Used in Disability Claims
Technology is now used across many parts of the disability claims process. Some tools are meant to speed up review. Some tools are meant to reduce fraud.
Some tools are meant to make filing easier for claimants and providers. These systems can improve access in real situations, but they can also create new problems when accessibility, design, or human oversight are weak.
AI and Machine Learning in Claims Review
AI and machine learning are now being used more often in insurance claims systems. One use is fraud detection. In Canada, insurers are pooling claims data and applying AI models to identify suspicious patterns across very large volumes of records.
The Canadian Life and Health Insurance Association has reported that insurers paid C$36.6 billion in health claims in 2023, and the association is involved in an AI program intended to detect suspicious claims earlier.
AI can also be used for claim triage and review support. A system may flag a file for fast handling, identify missing pieces of documentation, or sort cases by risk indicators. In theory, this can reduce manual burden and move some files faster through early review stages. A routine file with complete records may move forward more quickly when software handles the first round of checks.
The concern is that AI does not remove risk. It shifts risk into a different form. Insurers and claims administrators still have to deal with high implementation costs, legal concerns, ethical concerns, and questions about bias.
A 2025 RGA review said that insurers are interested in AI but also cautious about using it in disability claims. One reason is the fear that opaque decision systems may affect claimants unfairly. A claimant who does not understand why a file was flagged or delayed may have no clear way to challenge the logic behind it.
Telehealth and Remote Assessment
Telehealth expanded rapidly during the COVID 19 period, and it continues to affect how medical evidence is created and shared. CDC data showed that telehealth visits in the United States rose 50% in early 2020 compared with 2019, with a spike of 154% in late March 2020. That shift changed how many patients interact with doctors, therapists, and rehabilitation providers.
For disability claimants, telehealth can reduce travel and improve access to clinicians. A claimant in a rural area may be able to speak with a specialist online instead of traveling long distances. A person with mobility limits may be able to attend follow up appointments, therapy sessions, or rehabilitation reviews from home. These visits can still produce records that support a claim.
Telehealth also creates a more regular record of treatment in some cases. A patient can attend more appointments because the logistics are easier. That can help when insurers or government programs want documented proof of ongoing symptoms, treatment attempts, or medical monitoring.
The problem is that remote access is not equal access. Telehealth platforms still need captioning, screen reader support, interpreter access, and other accommodations. In the United States, the ADA applies to accessibility in these contexts, but real world compliance still falls short in many systems. A person may technically have access to a remote appointment but still struggle to use the platform if the interface is poorly built or if the accommodation is missing.
Digital Documentation and Electronic Signatures
Claims systems have steadily moved from paper records to digital files. Claimants can now upload medical reports, prescriptions, supporting statements, and identity documents through online systems instead of mailing paper copies. Doctors and claimants can also use electronic signatures for authorizations and forms.
This can reduce delays directly. A document can be uploaded the same day it is signed. A reviewer can access it without waiting for physical delivery. A clinic can send a file faster. A claimant can store copies of every uploaded record and refer to them later if the file is questioned.
Digital documentation also changes the timing of claims communication. A claimant no longer needs office hours to send a form. An upload can happen at any time. Some systems also let users check claim status online instead of waiting for a mailed update or a call center response.
The weakness is that digital submission still depends on functioning technology and user confidence. A person may have poor internet access. A person may not be comfortable scanning files, compressing documents, or checking file type limits.
Some disabled users also face direct barriers with touchscreens, mobile keyboards, or interface controls. Survey data in Canada show that 12% of Canadians with disabilities report difficulty using touchscreens. A failed upload or a timed out session can become a serious problem when deadlines are close.
Claim Portals and Mobile Apps
Most large insurers now provide claim portals or mobile apps for policyholders and claimants. These tools usually let users file a new claim, upload documents, track progress, receive notices, and sometimes communicate through built-in chat or secure messaging.
The practical appeal is clear. A portal can give a claimant a checklist, show what is still missing, and send a notice when a document is received. A mobile app can reduce mailing delays and cut down on repeated phone calls. A person who is already managing treatment, pain, fatigue, or work loss may find it easier to submit everything from one account.
The problem appears when these portals are not designed with accessibility in mind. A user with low vision may struggle if the portal has weak contrast, poor screen reader labeling, or missing alt text. A user with a cognitive disability may struggle if the process is cluttered, rushed, or confusing.
A user with hearing or speech limitations may face extra barriers if support depends on phone calls. A platform may promise self service, but self service breaks down when the interface excludes the user.
Technical glitches also remain a real issue. A file may appear uploaded but not attach correctly to the case. A browser may not support part of the system. A login process may fail repeatedly. A claimant may then need manual intervention, which removes the time savings that the portal was supposed to provide.
What Technology Has Improved and What It Still Has Not Fixed
Technology has changed disability claims, but the results are mixed. Some improvements are visible. Automation can route claims more quickly. Telehealth can make medical evidence easier to gather. Digital records can move faster than paper. Portals can give users more visibility into what is happening with their file.
At the same time, better technology does not automatically produce better claim outcomes. In the United States, more claims have been moving through the system, and the backlog has been shrinking from peak levels, but approval rates have still declined. That means faster movement through a system does not always mean a better result for claimants. Staffing levels, policy rules, evidentiary standards, and review culture still matter.

Accessibility and User Experience Remain Weak Points
Accessibility is still one of the biggest limits in digital claims systems. A portal may meet technical requirements on paper but still be hard to use in practice.
A screen reader user may get stuck on unlabeled fields. A claimant with cognitive fatigue may lose progress because of short timeouts. A deaf claimant may find that video communication lacks captioning. These are not small design issues. These issues affect whether a person can complete the process at all.
Statistics from Canada show how common digital barriers still are. A reported 17% of Canadians with disabilities say online activities create difficulties. That means the same systems that are supposed to reduce friction can create a new layer of friction for a large group of users. A claim system that moves fully online without proper accommodations may become less accessible than the paper system it replaced.
Privacy and Security Concerns Are Increasing
The more disability claims move online, the more sensitive health and identity information moves online as well. That creates real privacy and security exposure. The healthcare sector faced hundreds of cyberattacks in 2024. In the United States alone, 491 large-scale healthcare breaches were reported between January and September 2024. One of the most widely discussed incidents involved Change Healthcare, a claims processor, where about 190 million records were exposed.
When a breach affects a claims processor, the damage can extend beyond privacy. Processing can slow down. Records may become unavailable. Claimants may worry about stolen medical details, Social Security numbers, or insurance information. Laws such as HIPAA in the United States and PIPEDA in Canada require strong privacy protections and breach reporting, but legal rules do not remove the risk created by weak security or human error.
Accessibility and UX Challenges
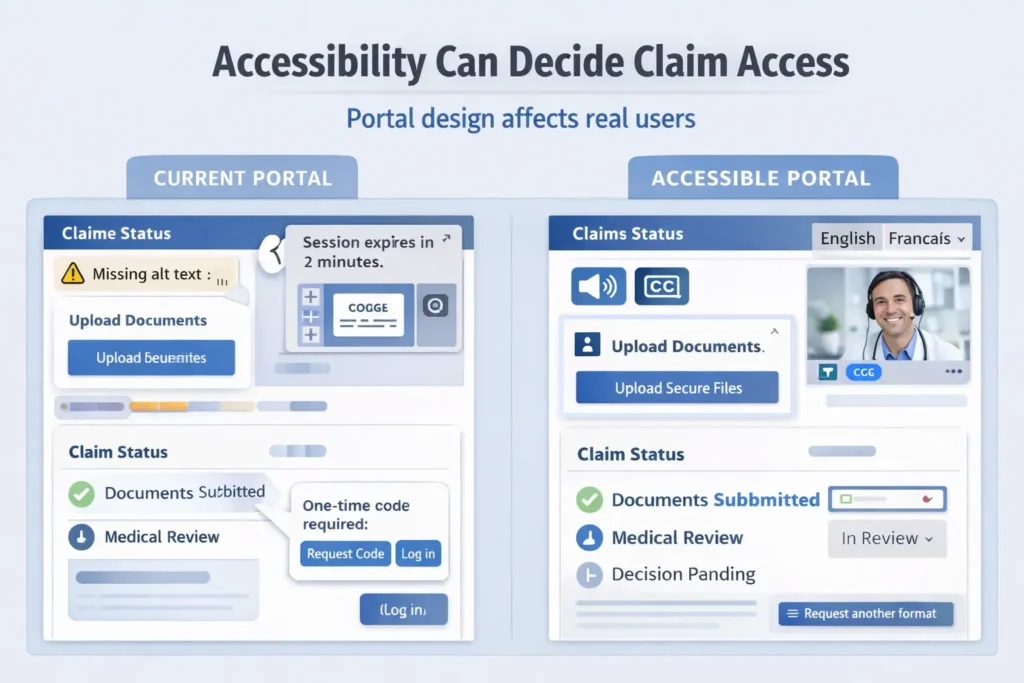
Technology in disability claims only works well when people can actually use it. Many people with disabilities still face problems with digital interfaces during the claims process. A claims portal with short session time limits or a crowded layout can stop a user from finishing a form or uploading documents on time.
Some barriers look small at first but still create real access problems. Missing alt text on images can make navigation harder for screen reader users. Limited language support can make instructions harder to understand. Two factor authentication can create barriers for people with hearing, vision, or cognitive impairments. Because of this, many industry groups continue to stress WCAG based design and direct user testing with disabled claimants. When a form or website feels inaccessible, a claimant should ask for another format or request support from an advocate.
When Technology Fails: The Role of Disability Lawyers
Digital systems can reduce paperwork, but they do not remove every problem from the claims process. Automatic denials, failed uploads, and system errors can still leave valid claims delayed or stuck without a clear explanation. In these situations, legal support can become necessary.
A disability lawyer in Toronto can review policy language, ask for human review, and handle appeal related paperwork when the digital system is not enough. A lawyer can also step in when an insurer’s portal classifies a claim incorrectly because of a technical or data related error. Technology can support a claim, but it cannot fully replace professional advocacy when the process becomes unclear or unfair.
When Human Help Still Matters
Technology can move information, sort files, and automate some tasks. Technology cannot fully replace human judgment when a claim becomes complicated, unfairly delayed, or wrongly denied.
A system error may misclassify a document. A portal may lose an upload. An automated review step may trigger a denial that the claimant does not understand. In those situations, the file usually needs human review, direct advocacy, or legal intervention.
A disability lawyer or claims advocate can step in when the process stops making sense. That person can review policy language, handle appeals paperwork, challenge procedural mistakes, and push for a real explanation when an insurer or agency response is unclear. Technology may support the process, but it does not remove the need for trained people when the process fails.
Technology Comparison Table
| Technology | Use in disability claims | Main benefit | Main risk or limit |
|---|---|---|---|
| AI and machine learning | Fraud detection, claim triage, risk scoring | Faster pattern review and early flagging of files | Bias concerns, weak transparency, and high cost |
| Telehealth | Remote exams, therapy, follow-ups | Better access for remote users and mobility limited users | Internet dependence and missing accommodations |
| Digital documents and e-signatures | Uploading forms, records, and signed authorizations | Faster submission and easier record storage | Upload failures, digital skill barriers, and security exposure |
| Claim portals and mobile apps | Filing claims, tracking status, receiving updates | More visibility and round the clock access | Accessibility barriers, login issues, and system glitches |
Practical Steps Claimants Can Take
A disability claim is still easier to manage when the claimant treats every digital action as something that may need proof later. That means keeping copies, checking upload confirmations, and following up when a system does not respond.
- A claimant should review every form and medical record before submission.
- A claimant should keep copies of uploaded records and confirmation emails.
- A claimant should monitor portal updates and follow up when a file stops moving.
- A claimant should ask for an accommodation early if a website, app, or remote platform creates access barriers.
Privacy also needs attention during the claims process because health information moves through many digital channels now.
- A claimant should use secure portals or other approved channels when sharing documents.
- A claimant should report suspicious emails, account activity, or possible data leaks quickly.
Reflection on Where the System Stands
Technology has made disability claims more digital, more connected, and in some cases faster. It has also made the process more dependent on good interface design, reliable infrastructure, strong security, and human oversight. A digital claims system can reduce delay for one claimant and create a new barrier for another claimant at the same time.
That is why the real issue is not only whether claims systems use technology. The real issue is how that technology is built, how it is supervised, and whether disabled claimants can actually use it without losing access, privacy, or fairness during the process.
FAQs
Does technology always make disability claims faster?
Technology can speed up parts of the process, such as document submission, file routing, and status tracking. A faster system step does not always mean the full claim is resolved faster. Staffing limits, medical evidence rules, and review standards still affect the final timeline.
Can telehealth records be used in a disability claim?
Telehealth records can support a disability claim when they document symptoms, treatment, follow ups, rehabilitation, or clinician observations. The value of those records still depends on the rules of the insurer or government program and on how complete the records are.
What should a claimant do if a portal or app is hard to use?
A claimant should ask for an accommodation as early as possible. That may include another format, extra support, or another submission method. A claimant should also keep records of the access problem in case the issue affects a deadline or a missing document dispute.
When should someone get legal help with a disability claim?
A claimant should consider legal or professional help when a claim is denied without a clear explanation, when a file is stalled for a long period, when documents appear to be lost, or when the system keeps producing errors that block a fair review.